
This post originally appeared in the Health Affairs blog.
By: Mark B. McClellan, Mark D. Smith, Thomas Buckingham
April 3, 2019
Health care spending is projected to grow to 19.4 percent of gross domestic product (GDP) by 2027, and big gaps in quality and access to care persist. This has motivated payers and providers to implement alternative payment models (APMs) to enable higher-value care. There is bipartisan agreement, reflected in the Medicare Access and CHIP Reauthorization Act (MACRA) and actions by Republican and Democratic administrations, that moving away from fee-for-service (FFS) towards value-based payment is critical.
The Health Care Payment Learning & Action Network (LAN), a multi-stakeholder-driven public-private partnership, was established by the Centers for Medicare and Medicaid Innovation (CMMI) in 2015 to accelerate this transition. With broad collaboration from public and private payers, the LAN has used its hallmark Alternative Payment Model (APM) Framework to categorize U.S. health care payments and identify the percentage of payments made through shared savings/risk models, episode-based payment models, and population-based models.
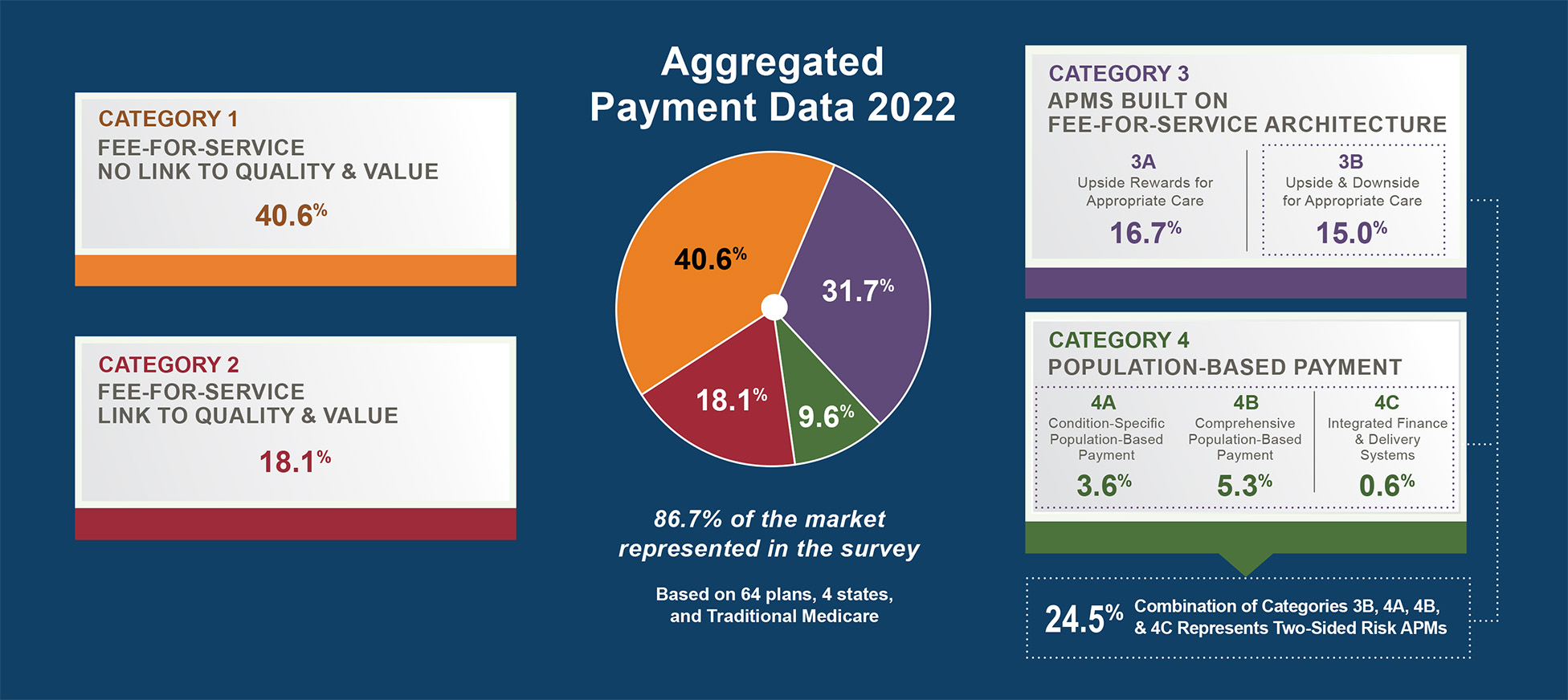
The LAN found that, in 2015, 23 percent of all health care payments were tied to APMs, or Categories 3 and 4 payment models as defined by the LAN Framework. The most recent APM measurement effort determined that 34 percent of health care payments in 2017 were tied to an APM; 12.5 percent of all payments were linked to downside risk models.
The growth in payments tied to APMs is encouraging. However, progress has been difficult, and the field has not moved as far or as fast as is necessary (and possible) to improve care and lower costs.
The Roadmap
To address this challenge, the LAN has developed a Roadmap for Driving High Performance in Alternative Payment Models (the “Roadmap”), an interactive, web-based implementation guide that public and private payers can use to work with providers, purchasers, patients, consumers, and others. The Roadmap was developed from research and interviews with 13 providers and nine payers — including large and small commercial payers and the Centers for Medicare & Medicaid Services (CMS) — representing ten different successful population-based and episode-based payment models.
The Roadmap offers users a robust set of promising practices organized around three domains—APM Design, Payer-Provider Collaboration, and Patient-Centered Care—that provide real-world guidance for organizations seeking to design, operate, and scale APMs. The interactive design enables Roadmap users to access specific resources relevant to their own context and challenges.
Identify And Engage Provider Champions
Payers strategically approach the APM as a payer-provider partnership by identifying and engaging clinical and executive champions in leadership positions, both within practices and across the entire provider organization. Subsequently, they seek to maintain close payer-provider connection to provide support for the APM and ensure alignment, engagement, and a shared understanding of what it will take to be successful.
Engage Patients At All Points Along The Design And Implementation Process
Some payers in both population-based and episode-based payment models require providers to have deliberate discussions with patients in the APM through care compacts, which outline the provider’s role (e.g., coordinating care) and patients’ responsibilities in their care (e.g., medication adherence). Payers in multi-payer models are also engaging patient representatives in APM design and implementation approaches, and they have found that patient input has improved APM operations.
Utilize Collaborative Strategies
Payers use collaborative strategies, such as multidisciplinary care management teams to engage patients in local communities and provider advisory councils to ensure buy-in from providers on APM design and redesign. The collaborative nature of these efforts allows payers to engage critical stakeholders and understand how design elements will affect those who deliver and receive care.
The Roadmap also reflects how providers are facing the challenges and opportunities in APM design and implementation.
Misalignment in APM design and data-sharing across payers creates administrative burdens for small practices and large provider organizations. Smaller practices value the reduced burden associated with aligned approaches across payers. Where there is a lack of alignment, while larger provider organizations can reduce administrative burden by negotiating alignment on APM components (e.g., quality measure sets).
Separate Provider-Level And Patient-Level Data
Providers find provider-level performance reports and patient-level “gap” reports (so named because they identify gaps in patient care) more actionable than reports that aggregate patient- and provider-level data.
Use Shared Decision-Making, But Not One Size Fits All
While payers and providers support shared decision-making between providers and patients in patients’ care, providers generally disagree with standardized shared decision-making requirements across all patients because they consider them unnecessarily burdensome and not desired by patients.
Support Patients Social Needs
Providers support patients who cannot afford to eat a healthy diet through various methods, including direct support in applying for supplemental nutritional assistance, connecting patients to community resources, and providing targeted nutritional counseling and food directly. Providers have identified various methods to support patients without reliable transportation, including the use of flexible funds (e.g., global payments, care management fees) to purchase a car for nurses to provide home care.
Together, these promising practices give payers and providers access to broader experience and insight into each other’s perspective on what is needed to successfully collaborate through APMs. The Roadmap illustrates where payers and providers have found common ground, and it demonstrates that pathways toward payment transformation are available no matter where one is in the process of APM design and implementation.
A final insight from the Roadmap is that context matters. Opportunities for change, approaches to design and implementation, and pace of adoption vary depending on a number of factors, such as the unique characteristics of local markets. The LAN hopes that a wide audience can use the Roadmap as a tool for payment and care delivery transformation.
Next Steps
While we believe that the Roadmap is an important step, we recognize that there is still much to learn to accelerate progress on payment reform. The Roadmap concludes with a section that addresses potential ideas and strategies for moving forward in additional areas, including quality measurement, patient engagement, benefit designs that support APMs, and opportunities for multi-payer alignment and synergies across many of these areas.
We look forward to your use of and feedback on the Roadmap, as this living resource will help inform and drive the activities of the LAN moving forward. We encourage users to provide feedback and share their experiences.















 Emily DuHamel Brower, M.B.A., is senior vice president of clinical integration and physician services for Trinity Health. Emphasizing clinical integration and payment model transformation, Ms. Brower provides strategic direction related to the evolving accountable healthcare environment with strong results. Her team is currently accountable for $10.4B of medical expense for 1.6M lives in Medicare Accountable Care Organizations (ACOs), Medicare Advantage, and Medicaid and Commercial Alternative Payment Models.
Emily DuHamel Brower, M.B.A., is senior vice president of clinical integration and physician services for Trinity Health. Emphasizing clinical integration and payment model transformation, Ms. Brower provides strategic direction related to the evolving accountable healthcare environment with strong results. Her team is currently accountable for $10.4B of medical expense for 1.6M lives in Medicare Accountable Care Organizations (ACOs), Medicare Advantage, and Medicaid and Commercial Alternative Payment Models. Victor is the Chief Medical Officer for TennCare, Tennessee’s Medicaid Agency. At TennCare, Victor leads the medical office to ensure quality and effective delivery of medical, pharmacy, and dental services to its members. He also leads TennCare’s opioid epidemic strategy, social determinants of health, and practice transformation initiatives across the agency. Prior to joining TennCare, Victor worked at Evolent Health supporting value-based population health care delivery. In 2013, Victor served as a White House Fellow to the Secretary of Health and Human Services. Victor completed his Internal Medicine Residency at Emory University still practices clinically as an internist in the Veteran’s Affairs Health System.
Victor is the Chief Medical Officer for TennCare, Tennessee’s Medicaid Agency. At TennCare, Victor leads the medical office to ensure quality and effective delivery of medical, pharmacy, and dental services to its members. He also leads TennCare’s opioid epidemic strategy, social determinants of health, and practice transformation initiatives across the agency. Prior to joining TennCare, Victor worked at Evolent Health supporting value-based population health care delivery. In 2013, Victor served as a White House Fellow to the Secretary of Health and Human Services. Victor completed his Internal Medicine Residency at Emory University still practices clinically as an internist in the Veteran’s Affairs Health System. Tamara Ward is the SVP of Insurance Business Operations at Oscar Health, where she leads the National Network Contracting Strategy and Market Expansion & Readiness. Prior to Oscar she served as VP of Managed Care & Network Operations at TriHealth in Southwest Ohio. With over 15 years of progressive health care experience, she has been instrumental driving collaborative payer provider strategies, improving insurance operations, and building high value networks through her various roles with UHC and other large provider health systems. Her breadth and depth of experience and interest-based approach has allowed her to have success solving some of the most complex issues our industry faces today. Tam is passionate about driving change for marginalized communities, developing Oscar’s Culturally Competent Care Program- reducing healthcare disparities and improving access for the underserved population. Tamara holds a B.A. from the University of Cincinnati’s and M.B.A from Miami University.
Tamara Ward is the SVP of Insurance Business Operations at Oscar Health, where she leads the National Network Contracting Strategy and Market Expansion & Readiness. Prior to Oscar she served as VP of Managed Care & Network Operations at TriHealth in Southwest Ohio. With over 15 years of progressive health care experience, she has been instrumental driving collaborative payer provider strategies, improving insurance operations, and building high value networks through her various roles with UHC and other large provider health systems. Her breadth and depth of experience and interest-based approach has allowed her to have success solving some of the most complex issues our industry faces today. Tam is passionate about driving change for marginalized communities, developing Oscar’s Culturally Competent Care Program- reducing healthcare disparities and improving access for the underserved population. Tamara holds a B.A. from the University of Cincinnati’s and M.B.A from Miami University.


 Dr. Peter Walsh joined the Colorado Department of Health Care Policy and Financing as the Chief Medical Officer on December 1, 2020. Prior to joining HCPF, Dr. Walsh served as a Hospital Field Representative/Surveyor at the Joint Commission, headquartered in Oakbrook Terrace, Illinois.
Dr. Peter Walsh joined the Colorado Department of Health Care Policy and Financing as the Chief Medical Officer on December 1, 2020. Prior to joining HCPF, Dr. Walsh served as a Hospital Field Representative/Surveyor at the Joint Commission, headquartered in Oakbrook Terrace, Illinois.





