About HCPLAN
What is the Health Care Payment Learning & Action Network (HCPLAN)?
The HCPLAN is a collaborative network of public and private health care leaders working to accelerate the transition to value-based payment models and accountable care. The HCPLAN convenes stakeholders across the health care ecosystem, including payers, providers, purchasers, policymakers, patients, advocates, and researchers, to share insights and advance payment approaches that improve quality, affordability, and health outcomes.
What is the HCPLAN’s mission?
The HCPLAN works to advance a health care system that delivers high-quality care, a better patient experience, and improved health outcomes at a lower cost by increasing the adoption of value-based payment models.
What is the HCPLAN Executive Forum?
The HCPLAN Executive Forum (EF) is a leadership body composed of senior health care executives from across the public and private sectors who provide strategic guidance for the HCPLAN’s priorities and Initiatives. The EF helps shape the HCPLAN’s direction by identifying opportunities to accelerate value-based payment adoption and strengthen collaboration and innovation across the health care system.
Value-Based Payment & HCPLAN APM Framework
What is value-based payment?
Value-based payment refers to payment models that reward providers for delivering high-quality, efficient care rather than paying primarily for the volume of services delivered. These models often link payment to patient outcomes, care coordination, and cost management, helping improve quality while controlling health care spending.
What is accountable care?
Accountable care is centered on the patient and aligns their care team to support shared decision-making and to realize the highest achievable health outcomes for all through comprehensive, high-quality, affordable, longitudinal care. The HCPLAN developed the Accountable Care Curve as a resource to help stakeholders drive the adoption of accountable care through a four step framework: learning, investing, aligning, and transforming.
What are alternative payment models?
Alternative payment models (APMs) are payment approaches designed to move beyond traditional fee-for-service reimbursement. APMs encourage providers to deliver high-quality, coordinated, and cost-effective care by linking payment to performance, outcomes, or overall total cost of care.
What is the HCPLAN APM Framework?
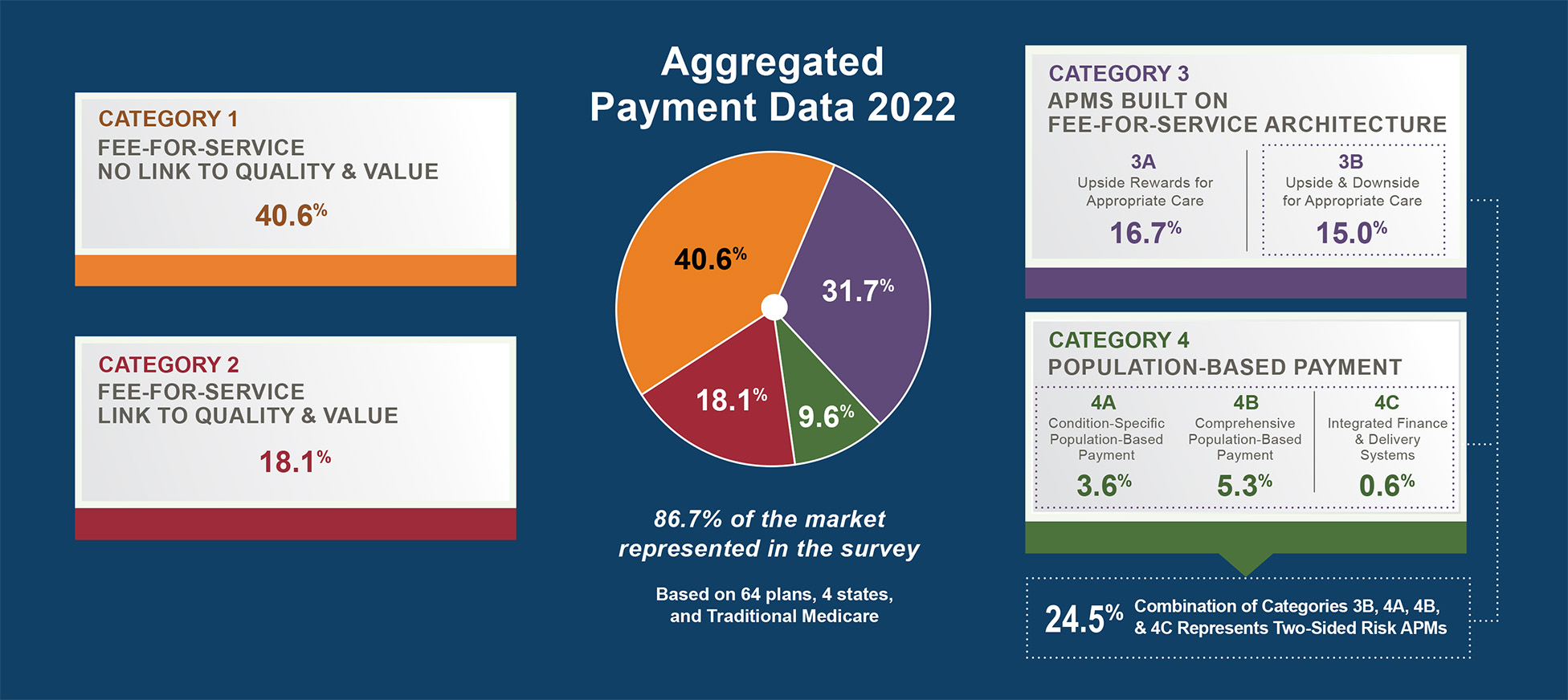
The HCPLAN APM Framework established a common vocabulary that categorizes health care payment models based on how closely they are tied to quality and value. The framework helps stakeholders track progress toward value-based payment adoption across the health care system.
HCPLAN Priority Initiatives
How did the HCPLAN determine its current priority initiatives?
These initiatives were designed to build on the prior work of the HCPLAN and in alignment with CMS Innovation Center’s Strategic Direction as well as emerging trends across the health care industry, ensuring the HCPLAN remains a leading, trusted voice in the health care ecosystem.
Each workgroup is championed by leaders in the public, private, and nonprofit sectors who are committed to advancing the adoption of APMs and driving value in the health care system. To drive the initiatives forward, the HCPLAN created four workgroups: Choice and Competition, Patient Empowerment, Evidence-Based Prevention, and Technology-Enabled Health Care.
How do the HCPLAN workgroups operate?
The HCPLAN workgroups were established as the vehicle to advance the priority initiatives by convening stakeholders from across the health care system to share expertise, discuss emerging challenges, and identify actionable solutions that accelerate adoption of value-based payment models. These collaborations help inform policy, industry best practices, and future HCPLAN priorities.
Measurement & Data
What are the HCPLAN’s goals for value-based payment adoption?
The HCPLAN has established goals to increase the share of U.S. health care payments tied to value-based models, particularly those that include downside financial risk, to support a more sustainable and patient-centered health care system.
What happened to the APM Measurement Effort?
In 2025, HCPLAN handed off the APM Measurement Effort to AHIP. Find the latest results here.
HCPLAN Participation & Resources
How can I get involved with the HCPLAN?
Interested individuals and organizations can sign up for the HCPLAN email listserv and follow us on LinkedIn and X. If you are working on any of the current initiatives areas, the HCPLAN would love to hear from you. You can get in touch here.
What resources does the HCPLAN provide?
The HCPLAN offers 2021-2025 measurement reports, frameworks, tools, and collaborative learning opportunities that help stakeholders understand trends, share best practices, and advance payment innovation. Check out all of these and more in our Resource Library and our Events page.















 Emily DuHamel Brower, M.B.A., is senior vice president of clinical integration and physician services for Trinity Health. Emphasizing clinical integration and payment model transformation, Ms. Brower provides strategic direction related to the evolving accountable healthcare environment with strong results. Her team is currently accountable for $10.4B of medical expense for 1.6M lives in Medicare Accountable Care Organizations (ACOs), Medicare Advantage, and Medicaid and Commercial Alternative Payment Models.
Emily DuHamel Brower, M.B.A., is senior vice president of clinical integration and physician services for Trinity Health. Emphasizing clinical integration and payment model transformation, Ms. Brower provides strategic direction related to the evolving accountable healthcare environment with strong results. Her team is currently accountable for $10.4B of medical expense for 1.6M lives in Medicare Accountable Care Organizations (ACOs), Medicare Advantage, and Medicaid and Commercial Alternative Payment Models. Victor is the Chief Medical Officer for TennCare, Tennessee’s Medicaid Agency. At TennCare, Victor leads the medical office to ensure quality and effective delivery of medical, pharmacy, and dental services to its members. He also leads TennCare’s opioid epidemic strategy, social determinants of health, and practice transformation initiatives across the agency. Prior to joining TennCare, Victor worked at Evolent Health supporting value-based population health care delivery. In 2013, Victor served as a White House Fellow to the Secretary of Health and Human Services. Victor completed his Internal Medicine Residency at Emory University still practices clinically as an internist in the Veteran’s Affairs Health System.
Victor is the Chief Medical Officer for TennCare, Tennessee’s Medicaid Agency. At TennCare, Victor leads the medical office to ensure quality and effective delivery of medical, pharmacy, and dental services to its members. He also leads TennCare’s opioid epidemic strategy, social determinants of health, and practice transformation initiatives across the agency. Prior to joining TennCare, Victor worked at Evolent Health supporting value-based population health care delivery. In 2013, Victor served as a White House Fellow to the Secretary of Health and Human Services. Victor completed his Internal Medicine Residency at Emory University still practices clinically as an internist in the Veteran’s Affairs Health System. Tamara Ward is the SVP of Insurance Business Operations at Oscar Health, where she leads the National Network Contracting Strategy and Market Expansion & Readiness. Prior to Oscar she served as VP of Managed Care & Network Operations at TriHealth in Southwest Ohio. With over 15 years of progressive health care experience, she has been instrumental driving collaborative payer provider strategies, improving insurance operations, and building high value networks through her various roles with UHC and other large provider health systems. Her breadth and depth of experience and interest-based approach has allowed her to have success solving some of the most complex issues our industry faces today. Tam is passionate about driving change for marginalized communities, developing Oscar’s Culturally Competent Care Program- reducing healthcare disparities and improving access for the underserved population. Tamara holds a B.A. from the University of Cincinnati’s and M.B.A from Miami University.
Tamara Ward is the SVP of Insurance Business Operations at Oscar Health, where she leads the National Network Contracting Strategy and Market Expansion & Readiness. Prior to Oscar she served as VP of Managed Care & Network Operations at TriHealth in Southwest Ohio. With over 15 years of progressive health care experience, she has been instrumental driving collaborative payer provider strategies, improving insurance operations, and building high value networks through her various roles with UHC and other large provider health systems. Her breadth and depth of experience and interest-based approach has allowed her to have success solving some of the most complex issues our industry faces today. Tam is passionate about driving change for marginalized communities, developing Oscar’s Culturally Competent Care Program- reducing healthcare disparities and improving access for the underserved population. Tamara holds a B.A. from the University of Cincinnati’s and M.B.A from Miami University.


 Dr. Peter Walsh joined the Colorado Department of Health Care Policy and Financing as the Chief Medical Officer on December 1, 2020. Prior to joining HCPF, Dr. Walsh served as a Hospital Field Representative/Surveyor at the Joint Commission, headquartered in Oakbrook Terrace, Illinois.
Dr. Peter Walsh joined the Colorado Department of Health Care Policy and Financing as the Chief Medical Officer on December 1, 2020. Prior to joining HCPF, Dr. Walsh served as a Hospital Field Representative/Surveyor at the Joint Commission, headquartered in Oakbrook Terrace, Illinois.





