At AARP, we consistently hear two messages from our members about health care: 1) they are worried about ever-increasing costs; and, 2) they want to find a good doctor who will really listen to them and address their needs – something that, for many, has become a frustrating ‘Where’s Waldo’-type experience.
Unfortunately, health care costs are continuing to climb – particularly the cost of prescription drugs. A recent AARP study shows that retail prices for brand name prescription drugs widely used by older Americans rose by an average of 15.5% in 2015—almost 130 times faster than inflation. The average annual cost for one brand name drug used on a chronic basis now exceeds $5,800. Lowering the cost of prescription drugs is a big, ongoing focus for us at AARP.
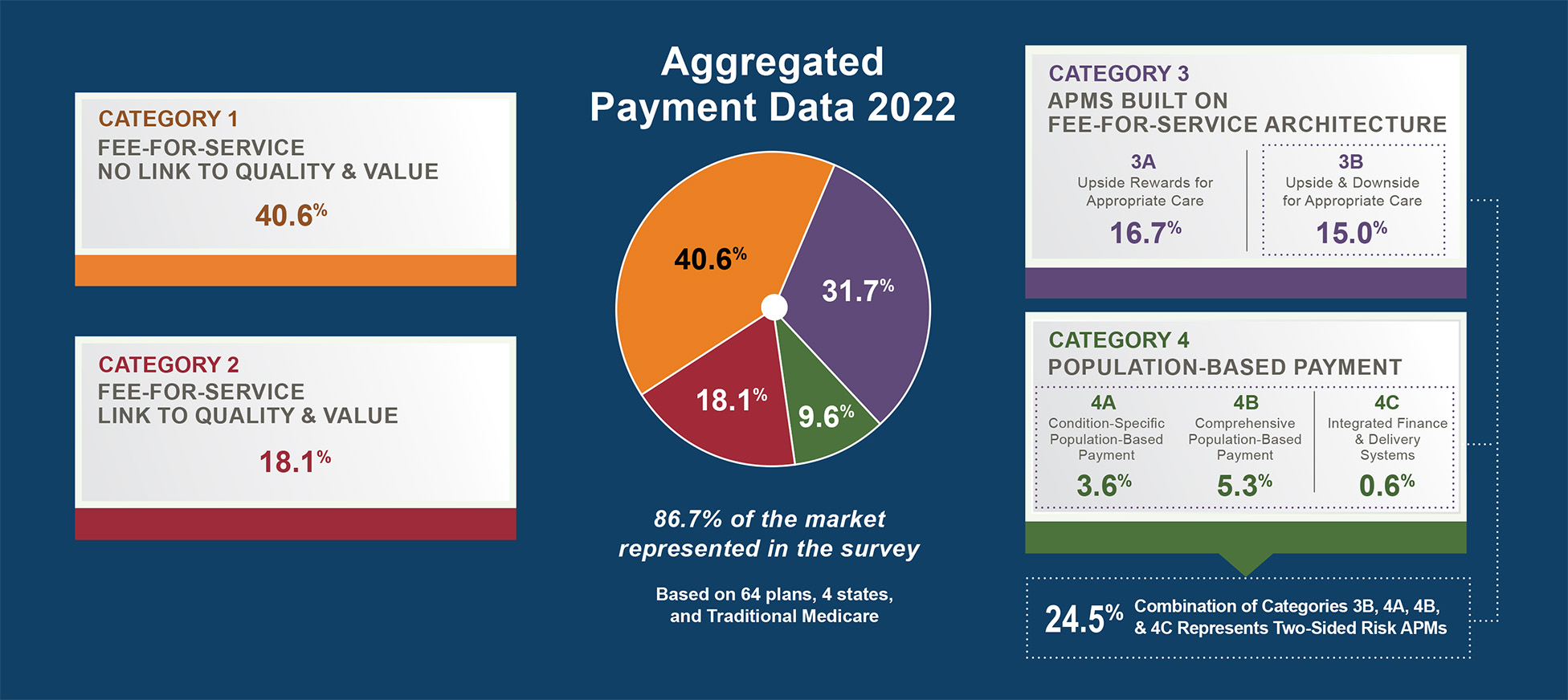
In the meantime, AARP is working with the Health Care Payment Learning and Action Network (LAN) on ways to speed the transformation of our health care system. We are especially focused on addressing the second concern – making health care more responsive to the needs of real people. There is a big movement underway to shift health care payments into alternative payment models (APMs) as a path to control costs and improve value for patients. The Medicare Access and CHIP Reauthorization Act of 2015 (MACRA), with provisions that begin this year, offers incentives to adopt APMs going forward. Certainly, we can find examples of payment models that reward quality of care more than expensive or unnecessary procedures. We can also point to health systems or plans that put the patient and their family caregiver’s needs first. But these examples are more the exception than the rule. It is urgent that consumers are part of this process to ensure we achieve patient-centered reform.
AARP and the LAN are working together to increase understanding of what “person-centered” care means and how it can help achieve three important goals: improve how care is delivered, put the needs of the person and family caregiver first, and use resources efficiently and prudently.
This is a cultural change that requires incorporating the patient perspective at every level – from including them when developing care plans to advising on how hospitals and provider groups are organized. As part of the LAN’s Consumer and Patient Affinity Group, AARP helped develop core principles to guide the transformation of health systems to become more person-centered: They are:
- Patients and their families must be in control of their care.
- Improving patient health must be the first and foremost commitment.
- Standards to evaluate provider performance and patient improvement should be meaningful, measureable, and accessible to everyone.
- Primary care is the foundation of better patient health and must be effectively coordinated with all aspects of patient care.
- There should be fair and equal access to high quality and innovative care.
- Modern tools and information technologies must be used to effectively manage and improve patient health.
- Provider compensation should be open, accessible, and available to everyone – and should balance the priorities to improve health while also reducing costs.
On the surface, these principles may seem intuitive, but too often they are overlooked in the herculean effort to overhaul payment and delivery systems.
A growing number of stakeholders across health care are voicing their support for the principle of person-centered health care delivery aimed at improving quality while reducing medical costs. There is much work to be done to bring the patient perspective into this culture shift. AARP is working to empower patients and consumers to ask the right questions, recognize value, and seek care that meets their personal or family’s needs. In fact, AARP’s December 2016 Bulletin devoted a special section to helping consumers understand the changing health care system and how they can be more engaged in their own care. True transformation – one that achieves better care, better outcomes, and lower costs — requires a concerted effort by everyone involved — doctors and hospitals, plans and insurers, employers, patients and their loved ones – and the LAN’s principles serve as a resource to inform payment reform design conversations.
AARP is doing its part to educate the public on how to be informed health care consumers, and we would like to hear how others are putting the principles into action.
Please note that guest blogs from Guiding Committee and Work Group members represent the views of the individual authors and do not represent official positions of the Guiding Committee, Work Groups, CAMH, or CMS.















 Emily DuHamel Brower, M.B.A., is senior vice president of clinical integration and physician services for Trinity Health. Emphasizing clinical integration and payment model transformation, Ms. Brower provides strategic direction related to the evolving accountable healthcare environment with strong results. Her team is currently accountable for $10.4B of medical expense for 1.6M lives in Medicare Accountable Care Organizations (ACOs), Medicare Advantage, and Medicaid and Commercial Alternative Payment Models.
Emily DuHamel Brower, M.B.A., is senior vice president of clinical integration and physician services for Trinity Health. Emphasizing clinical integration and payment model transformation, Ms. Brower provides strategic direction related to the evolving accountable healthcare environment with strong results. Her team is currently accountable for $10.4B of medical expense for 1.6M lives in Medicare Accountable Care Organizations (ACOs), Medicare Advantage, and Medicaid and Commercial Alternative Payment Models. Victor is the Chief Medical Officer for TennCare, Tennessee’s Medicaid Agency. At TennCare, Victor leads the medical office to ensure quality and effective delivery of medical, pharmacy, and dental services to its members. He also leads TennCare’s opioid epidemic strategy, social determinants of health, and practice transformation initiatives across the agency. Prior to joining TennCare, Victor worked at Evolent Health supporting value-based population health care delivery. In 2013, Victor served as a White House Fellow to the Secretary of Health and Human Services. Victor completed his Internal Medicine Residency at Emory University still practices clinically as an internist in the Veteran’s Affairs Health System.
Victor is the Chief Medical Officer for TennCare, Tennessee’s Medicaid Agency. At TennCare, Victor leads the medical office to ensure quality and effective delivery of medical, pharmacy, and dental services to its members. He also leads TennCare’s opioid epidemic strategy, social determinants of health, and practice transformation initiatives across the agency. Prior to joining TennCare, Victor worked at Evolent Health supporting value-based population health care delivery. In 2013, Victor served as a White House Fellow to the Secretary of Health and Human Services. Victor completed his Internal Medicine Residency at Emory University still practices clinically as an internist in the Veteran’s Affairs Health System. Tamara Ward is the SVP of Insurance Business Operations at Oscar Health, where she leads the National Network Contracting Strategy and Market Expansion & Readiness. Prior to Oscar she served as VP of Managed Care & Network Operations at TriHealth in Southwest Ohio. With over 15 years of progressive health care experience, she has been instrumental driving collaborative payer provider strategies, improving insurance operations, and building high value networks through her various roles with UHC and other large provider health systems. Her breadth and depth of experience and interest-based approach has allowed her to have success solving some of the most complex issues our industry faces today. Tam is passionate about driving change for marginalized communities, developing Oscar’s Culturally Competent Care Program- reducing healthcare disparities and improving access for the underserved population. Tamara holds a B.A. from the University of Cincinnati’s and M.B.A from Miami University.
Tamara Ward is the SVP of Insurance Business Operations at Oscar Health, where she leads the National Network Contracting Strategy and Market Expansion & Readiness. Prior to Oscar she served as VP of Managed Care & Network Operations at TriHealth in Southwest Ohio. With over 15 years of progressive health care experience, she has been instrumental driving collaborative payer provider strategies, improving insurance operations, and building high value networks through her various roles with UHC and other large provider health systems. Her breadth and depth of experience and interest-based approach has allowed her to have success solving some of the most complex issues our industry faces today. Tam is passionate about driving change for marginalized communities, developing Oscar’s Culturally Competent Care Program- reducing healthcare disparities and improving access for the underserved population. Tamara holds a B.A. from the University of Cincinnati’s and M.B.A from Miami University.


 Dr. Peter Walsh joined the Colorado Department of Health Care Policy and Financing as the Chief Medical Officer on December 1, 2020. Prior to joining HCPF, Dr. Walsh served as a Hospital Field Representative/Surveyor at the Joint Commission, headquartered in Oakbrook Terrace, Illinois.
Dr. Peter Walsh joined the Colorado Department of Health Care Policy and Financing as the Chief Medical Officer on December 1, 2020. Prior to joining HCPF, Dr. Walsh served as a Hospital Field Representative/Surveyor at the Joint Commission, headquartered in Oakbrook Terrace, Illinois.





